Higher taxes on sugary drinks and unhealthy foods must be complemented by making healthy alternatives more accessible and affordable






Should a can of cola be taxed similarly to a pack of cigarettes? The Government of India now effectively thinks so. Under the new Goods and Services Tax (GST) rules, the tax on carbonated sugar-sweetened beverages has been raised to 40%, placing these drinks firmly in the country’s ‘sin goods’ category alongside tobacco and alcohol. The goal behind such sin taxes, more politely called health taxes, is to make unhealthy products more expensive so people consume less of them, while also generating revenue to offset the public health costs associated with their consumption.
India’s consumption patterns make the case for such measures particularly urgent. The country is experiencing a rapid rise in non-communicable diseases (NCDs) such as diabetes, cardiovascular disease, and obesity, which now account for around 60% of all deaths nationwide and have increased sharply over the past few decades. This trend is closely linked to changing lifestyles, including higher consumption of processed foods, sugary beverages, and diets high in salt and fat.
In many countries, these taxes are structured as specific levies based on sugar content or volume rather than just price, because the harm comes from how much people consume, not how much they spend.
India’s move to levy a higher tax rate on sugary beverages is broadly in line with the World Health Organization’s recommendations, which argue that higher taxes on tobacco, alcohol, and sugary drinks can reduce consumption while raising public revenue. Health taxes are typically applied to products linked to NCDs such as diabetes, heart disease, and obesity. They are designed not just to raise prices, but to change behaviour, encourage reformulation by manufacturers, and signal public health priorities. In many countries, these taxes are structured as specific levies based on sugar content or volume rather than just price, because the harm comes from how much people consume, not how much they spend.

Despite being widely implemented globally, how much do we really know about the effectiveness of these taxes? In this column, I take a look at current scientific evidence to highlight their potential and limitations.
A good idea in theory
Before I started writing this column, I emailed a colleague—a health economics professor—to ask his opinion about the effectiveness of such taxes. He responded optimistically and pointed me towards several recent studies suggesting that taxes on unhealthy food and drink can improve diets and reduce disease. At first glance, the evidence pointed towards a clear positive corelation between such taxes and improved health outcomes. But as I started reading the papers more carefully, I realised that most of the evidence did not come from observing what actually happened after taxes were introduced. Instead, much of it came from economic modelling.
This is not necessarily a problem, but it is important to understand what modelling means in this context. Much of what we know about health taxes comes from simulations that first estimate how consumers are likely to respond to price increases and then project how those changes in consumption might affect health outcomes. A large systematic review of health taxes in 2017 found that modelling was the most common research method used in this field, far more common than real-world evaluations of the actual taxes.
There are good reasons for this. Measuring how people respond to price changes in the real world is extremely difficult. When a government introduces a tax on sugary drinks or ultra-processed food, the price goes up, but many other things change at the same time. Companies change product sizes or recipes, supermarkets run promotions, new products appear, and people switch to cheaper alternatives that may or may not be healthier. Isolating the effect of the tax from all these other factors is methodologically hard, especially over long periods of time. Ideally, researchers would track the same households for years and observe exactly how their purchasing behaviour changes as prices change, but that kind of data is expensive to generate and often difficult to access, particularly in low- and middle-income countries.
It is relatively straightforward to show that people buy fewer taxed drinks when prices rise. It is much harder to show that they consume fewer calories overall or develop fewer chronic diseases as a result.
As a result, researchers often rely on models. Typically, they estimate how sensitive people are to price changes (i.e., what economists call price elasticity) and then simulate what would happen to consumption patterns and health outcomes if prices increased by a certain amount. In the Indian context, for example, one recent study used household consumption data to estimate how different income groups respond to food price changes and then used a microsimulation model to project the effects of higher taxes on foods high in fat, sugar and salt over the next 30 years. The researchers simulated changes in nutrient intake, body weight, and the incidence of diseases like diabetes and heart disease and then estimated the impact on healthcare costs. The results suggested that higher taxes could reduce disease and health spending over time, but these results depend heavily on assumptions about how consumers respond to prices, how companies respond to taxes, and how changes in diet translate into changes in health many years later.

This approach is common in countries where comprehensive real-world data is limited. Even where taxes have been implemented, such as sugar taxes in Mexico, the UK, and parts of Europe, the clearest evidence tends to come from purchases rather than health outcomes. It is relatively straightforward to show that people buy fewer taxed drinks when prices rise. It is much harder to show that they consume fewer calories overall or develop fewer chronic diseases as a result. Health outcomes take years to change, and by the time they do, many other factors have changed too.
Also read: Ultra-processed foods are reshaping our diets. Should we be worried?
Moral issues
The moral debate on health taxes is as complicated as the economic one. Opponents of health taxes often argue that such policies are paternalistic. The argument is that if adults choose to drink sugary beverages or eat unhealthy food, that is a personal choice, and governments should not interfere in private decisions. This view draws on a long liberal tradition in political philosophy that places a high value on individual autonomy and freedom of choice. From this perspective, health taxes are seen as governments acting like overbearing parents, nudging citizens toward ‘better’ behaviour whether they want it or not. Food industry lobby groups often amplify this line of argument to resist the introduction of such taxes, framing them as unjustified intrusions on personal freedom.
What looks like a free choice is often heavily influenced by the food environment people live in. Taxes, in this view, do not remove choice but alter the environment in which choices are made.
But public health ethics looks at the issue differently. The case for health taxes is not just that individuals make unhealthy choices, but that these choices are shaped by environments, marketing, pricing, and availability. In other words, what looks like a free choice is often heavily influenced by the food environment people live in. Taxes, in this view, do not remove choice but alter the environment in which choices are made.
There is also the question of who bears the costs. Diet-related diseases such as diabetes and heart disease place a large burden on public health systems, which means that the costs are shared by society, not just by the individual consuming sugary drinks. This creates what economists call a social cost, and one of the classic justifications for taxation is to make the price of a product reflect its true social cost.
At the same time, health taxes raise concerns about fairness. Critics often argue that these taxes are regressive, meaning they take up a larger share of income from poorer households, who also tend to consume more of the taxed products. Supporters, however, argue that lower-income groups also suffer disproportionately from diet-related diseases, meaning they may also benefit the most from reduced consumption.
Also read: In an age of food abundance, why does ‘hidden hunger’ hold India back?
The way forward
If health taxes are not a silver bullet, what else should governments do?
One of the most consistent findings in public health research is that taxes work best when they are part of a broader policy package rather than a standalone measure. Prices do influence behaviour, but so do many other things: what is available in school canteens, how food is marketed to children, how products are labelled, and what kinds of foods are subsidised by governments. In other words, the food environment matters as much as (and sometimes more than) individual willpower.
This is particularly important in countries like India, where diets are changing rapidly, and ultra-processed foods are becoming cheaper and more heavily marketed. Taxing sugary drinks and other unhealthy foods may reduce consumption, but it does not automatically make healthier food more accessible or affordable. An important difference between health taxes on tobacco and alcohol and health taxes on food is that consuming food (even if unhealthy) is not optional. People do not need cigarettes or alcohol to survive, but they do need nutrients. For many low-income households, cheap packaged foods and sweetened beverages are not just treats but an affordable source of calories, which means that if prices rise, more affordable and accessible alternatives must be made available.
An important difference between health taxes on tobacco and alcohol and health taxes on food is that consuming food (even if unhealthy) is not optional.
This makes it important to think about taxes and subsidies together. If governments raise taxes on sugary drinks and unhealthy foods, they could use that revenue to subsidise fresh produce and essential cereals, invest in businesses that produce healthier alternatives, improve school meal programmes, or invest in public health campaigns. In this approach, the goal is not just to discourage unhealthy consumption, but to actively make healthier diets more accessible.
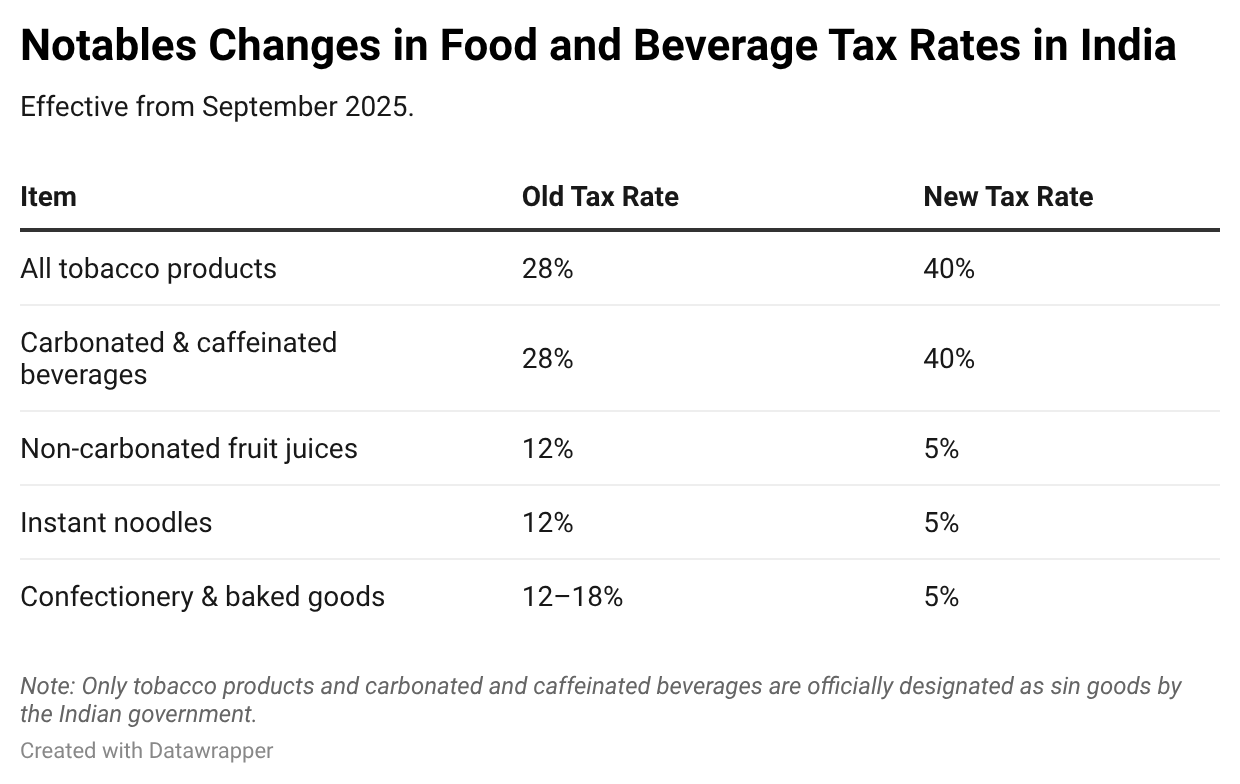
The GST overhaul of 2025 does reflect this policy direction to some extent. Taxes on suar-sweetened, carbonated, and caffeinated beverages have been raised to 40%, while rates on essential foods such as vegetables, fruits, and some nuts have been reduced from 12% to 5%. Some relatively healthier convenience foods, such as pasta and prepared soups, have also seen their tax rates lowered from 18% to 5%. However, other foods high in sugar, fats, and salt such as fruit juices, jams, ice cream, confectionery, instant noodles, packaged snacks, and even traditional Indian sweets, are now taxed at 5%, down from earlier rates of 12–18%. In several cases, these reductions have occurred despite calls to increase taxes on such products.
This perhaps points to the limits of relying on taxes alone. Around the world, there is a strong case for regulation beyond taxation. Restrictions on marketing to children, clear front-of-pack warning labels, limits on trans fats, and reformulation targets for salt and sugar have all been used in different countries. These policies often receive less attention than taxes, but in some cases, they may have a larger impact because they change the default choices available to consumers rather than relying on individuals to respond to price increases.
Ultimately, health taxes are best understood not as a solution on their own, but as one tool among many. The real challenge is not just to make unhealthy food more expensive, but to make healthy food more affordable and accessible.
Also read: Food fortification 101: Can foods built in with nutrients counter malnutrition, deficiencies?
Cover Art by Sharath Ravishankar
{{quiz}}
Explore other topics
References






.avif)




